How Alcohol Addiction Impacts Mental Health

Alcohol addiction, clinically known as Alcohol Use Disorder (AUD), is more than just excessive drinking. It’s a condition that deeply affects a person’s mind and life. In cities like Kolkata, where social drinking is often normalized during celebrations and stress is part of daily hustle, the line between casual use and dependency can blur quickly. What many overlook is how closely alcohol and mental health are connected. This blog explores that link, helping you understand the emotional and psychological effects, warning signs, and pathways to recovery, so you or your loved ones can take informed steps toward healing. What is Alcohol Addiction? Alcohol addiction, or AUD, is a chronic condition where a person struggles to control their drinking despite negative consequences. It goes beyond occasional drinking and develops into a physical and psychological dependence. Common signs include strong cravings, inability to limit intake, neglecting responsibilities, and continuing to drink despite health or relationship issues. In many local settings, weekend drinking or festive indulgence is common, but addiction is marked by loss of control and reliance. Risk factors include genetic predisposition, high-stress environments, trauma, and social influences. Many individuals don’t realize when casual drinking turns into dependency, which is why awareness and timely alcohol addiction treatment in Kolkata can make a crucial difference in preventing long-term mental health damage. Understanding Mental Health Mental health refers to our emotional, psychological, and social well-being. It influences how we think, feel, act, and handle stress in everyday life. Good mental health helps individuals cope with challenges, build relationships, and make sound decisions. However, conditions like anxiety, depression, and bipolar disorder are becoming increasingly common, especially in fast-paced urban environments like Kolkata. Work pressure, financial responsibilities, and social expectations can take a toll on emotional well-being. When mental health is compromised, it can affect sleep, appetite, productivity, and relationships. Understanding mental health is the first step toward recognizing how external factors, like alcohol, can either temporarily mask or significantly worsen these underlying conditions over time. The Link Between Alcohol and Mental Health Alcohol and mental health share a complex, two-way relationship. While some people turn to alcohol to cope with stress, anxiety, or emotional pain, excessive consumption can actually worsen these conditions. This is often called “self-medication,” where alcohol is used as a temporary escape. In reality, alcohol alters brain chemistry by affecting neurotransmitters responsible for mood regulation. While it may initially create a feeling of relaxation, over time it disrupts emotional balance. For someone already dealing with anxiety or depression, this can intensify symptoms. In many cases, untreated mental health issues lead to increased drinking, which further damages mental stability, creating a harmful cycle that becomes difficult to break without professional support. Short-Term Mental Health Effects of Alcohol Even short-term alcohol consumption can significantly impact mental health. After just a few drinks, individuals may experience mood swings, irritability, and lowered inhibitions. This often leads to impulsive decisions or risky behaviors that they might later regret. Alcohol can also trigger anxiety and panic attacks, especially once its effects begin to wear off. Many people report feeling more anxious the next day, a phenomenon often referred to as “hangxiety.” Sleep is also affected, as alcohol disrupts the natural sleep cycle, leading to poor rest and fatigue. In a busy city lifestyle, where people already struggle with stress, these short-term effects can quickly accumulate, making everyday functioning more difficult and emotionally draining. Long-Term Mental Health Consequences Prolonged alcohol addiction can have serious and lasting effects on mental health. One of the most common outcomes is depression, often accompanied by feelings of hopelessness and, in severe cases, suicidal thoughts. Chronic alcohol use can also lead to persistent anxiety disorders, making it difficult for individuals to cope with daily stress. Over time, alcohol affects brain function, leading to memory problems and cognitive decline. In extreme cases, individuals may experience alcohol-induced psychosis, which includes hallucinations and distorted thinking. These long-term consequences not only affect the individual but also their family and social life. Without timely intervention, the damage can become deeply rooted, making recovery more challenging but still possible with the right care and support. Co-Occurring Disorders: Dual Diagnosis Dual diagnosis refers to the presence of both alcohol addiction and a mental health disorder at the same time. For example, a person may struggle with depression, anxiety, or PTSD alongside alcohol dependency. This combination is more common than many realize. The challenge with dual diagnosis is that both conditions interact and worsen each other. Alcohol may temporarily ease emotional distress, but it ultimately intensifies mental health symptoms. This makes treatment more complex, as both issues need to be addressed simultaneously. Specialized care programs, like those offered by Sarathi Welfare Trust, focus on treating both addiction and mental health together, ensuring a more holistic and effective recovery process. Social and Emotional Impact Alcohol addiction doesn’t just affect the individual. It impacts their entire social circle. Relationships with family and friends often become strained due to behavioral changes, broken trust, and emotional distance. In many households, this leads to conflict, misunderstandings, and even isolation. Work performance can also suffer, resulting in job instability and financial stress. In a city like Kolkata, where family bonds and social reputation hold strong value, these challenges can feel overwhelming. Emotionally, individuals may experience guilt, shame, and a loss of self-esteem. Over time, this can create a sense of loneliness and hopelessness, making it even harder to seek help or break free from the cycle of addiction. Warning Signs to Watch For Recognizing the early signs of alcohol addiction can make a significant difference. Behavioral changes such as increased secrecy, neglecting responsibilities, or avoiding social interactions are common indicators. Emotionally, individuals may appear unstable, easily irritated, or withdrawn. A growing dependence on alcohol, such as needing it to relax or cope with stress, is another major red flag. Withdrawal symptoms like tremors, sweating, nausea, or anxiety when not drinking indicate physical dependence. If you notice these signs in yourself or someone close, it’s important to seek
The Science Behind Addiction Recovery and Rehabilitation
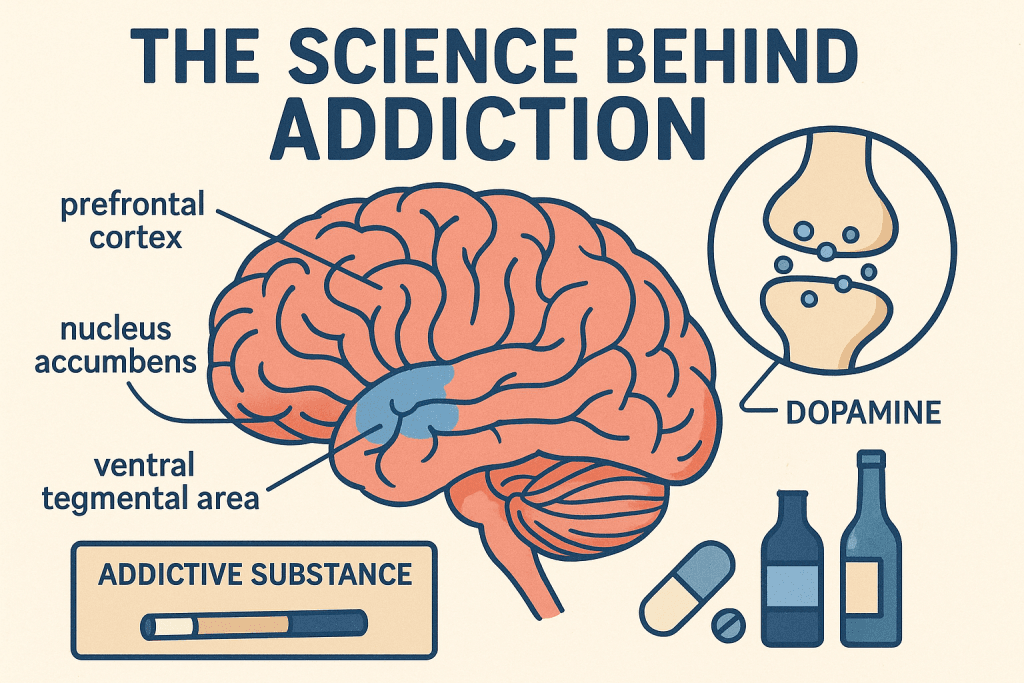
Hope flickers when science meets compassion in addiction recovery. Stories of struggle often hide powerful biology and brain chemistry. Addiction behaves like an illness, not a failure of character. Shame fades when medical facts replace myths and blame. Families suffer silently, unsure where to seek trusted help. The right support systems transform fear into structured healing journeys. Modern research reveals predictable patterns behind cravings and relapse. Treatment works best inside a professional rehab centre environment. Sarathi Welfare Trust follows evidence-based methods with humane care. Readers will explore brain science, risk factors, treatments, and recovery strategies here. What Is Addiction? Medical professionals classify addiction as Substance Use Disorder, a chronic brain condition. Condition disrupts control over substance use despite harmful consequences. Physical dependence occurs when the body adapts and demands the substance. Psychological addiction involves emotional reliance and compulsive behavioral patterns. Brain chemistry changes reduce impulse control and rational thinking ability. Reward circuits begin prioritizing substances over relationships, work, and health. Decision-making weakens as cravings overpower long-term judgment. Individuals may recognize harm yet feel unable to stop alone. Structured therapy and monitoring at a rehab centre in Kolkata significantly improve recovery outcomes. The Brain Science of Addiction Brain function changes dramatically during prolonged substance exposure. The reward system releases dopamine, creating pleasure and reinforcing survival behaviors. Addictive substances flood dopamine pathways far beyond natural stimulation levels. The brain starts associating substances with relief, motivation, and emotional comfort. The prefrontal cortex weakens, reducing judgment, planning, and impulse control. Amygdala becomes hypersensitive, intensifying stress, fear, and emotional reactions. The hippocampus stores powerful memories that link environments to substance experiences. Tolerance develops as the brain reduces sensitivity to repeated chemical surges. Higher quantities become necessary to achieve earlier pleasurable effects. Dependence forms when the brain adapts and functions poorly without substances. Withdrawal symptoms appear as the nervous system struggles to regain balance. Causes and Risk Factors Genetic makeup influences vulnerability to addictive behaviors across generations. Family history increases susceptibility through inherited neurochemical response patterns. Environmental exposure strongly shapes behavioral and emotional coping mechanisms. Childhood trauma often alters stress hormones and emotional regulation capacity. Peer groups can normalize risky experimentation and frequent substance use. Easy availability increases impulsive consumption and the likelihood of repeated behavioral reinforcement. Mental health disorders commonly coexist with addiction in complex cycles. Depression, anxiety, and PTSD intensify emotional discomfort and distress. Individuals may self-medicate symptoms without recognizing long-term neurological harm. Early screening and professional guidance at a rehab centre reduce compounded risks. The Recovery Process: What Happens in the Brain Brain recovery begins once substance use stops and stability improves. Neuroplasticity allows neural pathways to reorganize and regain functional balance. Healthy routines strengthen circuits responsible for motivation and emotional control. Cognitive clarity gradually improves over weeks and months of abstinence. Emotional regulation stabilizes as stress hormones return to manageable levels. Withdrawal triggers physical discomfort, anxiety, irritability, and sleep disturbances. Medical supervision ensures safety during detoxification and symptom management. Cravings emerge from conditioned memory circuits and environmental trigger exposure. Stress activates pathways previously linked to substance relief experiences. Structured therapy at a rehab centre teaches coping responses and relapse prevention. Evidence-Based Treatment Approaches Behavioral therapies reshape thinking patterns and emotional response systems. Cognitive Behavioral Therapy helps patients identify and replace harmful thought cycles. Dialectical Behavior Therapy strengthens emotional regulation and distress tolerance skills. Motivational Interviewing builds internal commitment toward sustainable lifestyle changes. Medication-Assisted Treatment reduces withdrawal severity and persistent craving intensity. Methadone stabilizes opioid receptors and prevents extreme physiological reactions. Buprenorphine partially activates receptors, reducing the risk of misuse and discomfort. Naltrexone blocks euphoric effects, discouraging repeated substance consumption. Holistic therapies complement medical treatment and improve overall well-being. Mindfulness practices reduce stress and improve present-moment awareness. Exercise restores natural dopamine balance and enhances mood stability. Comprehensive programs inside a rehab centre integrate therapy, medication, and lifestyle rebuilding. The Role of Rehabilitation Programs Rehabilitation programs provide structured environments designed for focused recovery. Inpatient rehabilitation removes individuals from triggers and harmful surroundings. Patients receive continuous medical supervision and psychological care. Daily schedules promote discipline, therapy participation, and healthy habit formation. Outpatient programs offer flexibility for work, education, and family responsibilities. Regular counseling sessions ensure continued accountability and progress tracking. Community recovery groups strengthen emotional resilience through shared experiences. Peer discussions reduce isolation and normalize recovery struggles. Group accountability encourages consistency and responsible decision-making habits. Alcoholics Anonymous supports sobriety through structured steps and sponsorship systems. Narcotics Anonymous offers community-based healing for substance dependence challenges. SMART Recovery emphasizes scientific self-management and cognitive skill development. Sarathi Welfare Trust is a reliable rehab centre in Kolkata with compassionate professionals and evidence-based care. It encourages long-term lifestyle rebuilding beyond detoxification phases. Technology and Innovation in Addiction Treatment Technology transforms accessibility and personalization in modern recovery programs. Telehealth counseling connects patients with specialists regardless of geographic limitations. Mobile recovery applications track habits, moods, triggers, and therapy goals. Wearable devices monitor heart rate variability and physiological stress signals. Real-time alerts help individuals manage emotional spikes proactively. Artificial intelligence analyzes behavioral patterns and predicts potential relapse risks. Digital tools complement structured therapy provided inside a rehab centre setting. Challenges in Recovery Recovery journeys often include setbacks that require patience and resilience. Relapse does not signal failure but indicates treatment adjustment needs. Social stigma prevents many individuals from seeking timely professional help. Discrimination affects employment opportunities and confidence in community reintegration. Limited access to quality treatment delays early intervention efforts. Financial burdens and family responsibilities complicate long-term therapy commitments. Supportive environments and guidance from a rehab centre reduce these recovery barriers. Preventing Relapse: What Science Recommends Relapse prevention begins with identifying personal, emotional, and environmental triggers. Patients learn coping mechanisms to manage stress without harmful behaviors. Structured routines reduce impulsive decisions and promote mental stability. Healthy sleep cycles improve emotional regulation and cognitive clarity. Regular exercise strengthens mood balance and reduces anxiety symptoms. Long-term therapy reinforces behavioral strategies and accountability systems. Ongoing monitoring ensures early intervention when warning signs reappear. The Future of Addiction Science Neuroscience continues to uncover detailed mechanisms behind
Inside Addiction Counselling: Step-by-Step Guide To Therapy And Recovery

Behavioural therapy counselling is a professional approach planned to help individuals overcome substance abuse, behavioural issues, or compulsive habits. It provides guidance, support, and practical tools to manage addiction while improving mental and emotional well-being. Understanding what happens during addiction counselling can ease fears and encourage people to seek help. What Is Addiction Counselling? It is a structured program that helps individuals identify, manage, and overcome addictive behaviours. Counsellors work with clients to understand triggers, build coping skills, and create personalized recovery plans. It’s not just therapy; it’s a comprehensive approach to support lasting change. What Happens During An Addiction Therapy Session? Recovery coaching is a structured process that helps individuals understand their addiction, develop coping strategies, and work toward recovery. Here is what it includes: Step 1: Assessment The first session focuses on understanding your addiction history, personal challenges, and triggers. The counsellor gathers essential information to create a personalized plan. This evaluation helps build trust, clarifies goals, and sets the foundation for an effective recovery journey. Step 2: Goal Setting Together with your counsellor, you define clear short-term and long-term goals. Goals may include reducing substance use, managing cravings, or improving emotional well-being. Setting objectives provides direction, motivation, and measurable milestones for tracking progress throughout therapy. Step 3: Therapy Sessions Core therapy sessions use behavioural techniques to address addictive behaviours. Counsellors guide clients through coping strategies, problem-solving skills, and managing triggers. Sessions are interactive, allowing individuals to explore underlying issues and practice new habits in a safe, supportive environment. Step 4: Treatment Steps After therapy, a structured plan is created to support recovery. This includes daily routines, relapse prevention strategies, and practising healthy habits. Following these steps consistently helps clients develop stability, resilience, and the skills needed to maintain long-term sobriety. Step 5: Recovery Process Recovery is gradual and requires commitment. Counsellors assist clients in monitoring progress, addressing challenges, and staying motivated. Emphasizing patience and consistency, this phase reinforces positive changes, helps prevent relapse, and builds confidence in the client’s ability to sustain recovery. Step 6: Addiction Support Ongoing support ensures recovery continues beyond sessions. Counsellors provide follow-ups, access to support groups, and resources to prevent relapse. Regular guidance, encouragement, and connection to a support network strengthen resilience and promote a healthier, addiction-free life. Common Challenges During Counselling Facing challenges is normal in addiction recovery. Understanding these obstacles helps you stay committed and navigate the process with confidence. Counsellors provide guidance, strategies, and support to overcome setbacks. Cravings and urges – Strong temptations to return to addictive behaviour. Guilt and shame – Feeling regret or embarrassment about past actions. Frustration and impatience – Progress can feel slow or overwhelming. Relapse fears – Anxiety about slipping back into old habits. Emotional ups and downs – Mood swings or stress can challenge recovery. Why Seeking Recovery Guidance Could Change Your Life? Recovery coaching is a step-by-step journey combining therapy, supportive steps, and ongoing support. Understanding the process helps clients feel prepared and confident. With professional guidance, anyone struggling with addiction can take the first step toward recovery and a healthier life. Seeking addiction counselling is not just about quitting habits but about learning skills for a lasting, fulfilling recovery. If you or your loved ones need help, we are here!
